ROCKEFELLER NEUROSCIENCE INSTITUTE RESEARCH
RNI RESEARCH BY THE NUMBERS, 2023
ACTIVE AWARDS
(in millions)
PEER-REVIEWED
PUBLICATIONS
CLINICAL RESEARCH
STUDIES
FIRST-IN-HUMAN STUDIES
(SINCE 2018)
SEVEN RESEARCH UNITS
Multidisciplinary bench to bedside research that pushes the boundaries of clinical innovation.
Children’s Neuroscience Center of Excellence
RNI Innovation Center
RNI INNOVATION CENTER
LEADING DISCOVERY
The RNI Innovation Center research team is a dedicated multidisciplinary group of clinicians, scientists, engineers, clinical trial specialists, and research staff focused on translational clinical trials. This team partners with academic, industry, and government partners to rapidly deploy new technologies to facilitate patient care and improve the lives of people suffering from neurological and behavioral health conditions.
Pictured is Blair Ellison, the world’s first patient to receive monoclonal antibody treatment with blood-brain barrier opening, is pictured with the RNI team following his first focused ultrasound treatment.


RNI receives funding to expand research and treatment for food addiction and PTSD
The West Virginia University Rockefeller Neuroscience Institute (RNI) will initiate first-in-the-world clinical research studies using focused ultrasound neuromodulation to treat food addiction, post-traumatic stress disorder (PTSD), and other conditions, thanks to a $2 million supplemental appropriation approved during a recent special session of the West Virginia Legislature.
The funding will allow the RNI to expand upon its current world-leading research using focused ultrasound technology to treat Alzheimer’s disease, substance use disorder, and other conditions.
Focused Ultrasound for Alzheimer’s
Researchers at RNI’s innovation center have been at the forefront of applying Focused ultrasound (FUS) with microbubbles to open the blood-brain barrier (BBB) in patients with Alzheimer’s disease and are now pioneering the combination of FUS with anti-beta amyloid antibodies. These antibodies specifically target the beta-amyloid plaques, a hallmark of Alzheimer’s disease, potentially improving their removal from the brain.
This targeted approach holds immense promise for treating the root cause of Alzheimer’s, not just managing its symptoms. The success of FUS technology, particularly RNI’s advancements, opens doors to treating a vast array of neurological diseases once deemed untouchable. The potential applications hold immense promise for revolutionizing neuroscience.
Visit ClinicalTrials.gov for trial details
Download a fact sheet
LEARN MORE:
- Ultrasound Blood–Brain Barrier Opening and Aducanumab in Alzheimer’s Disease – New England Journal of Medicine
- Battling Alzheimer’s through Better Access to the Brain – Scientific American Blog Network
- Focused ultrasound-mediated blood-brain barrier opening in Alzheimer’s disease: long-term safety, imaging, and cognitive outcomes
- Noninvasive hippocampal blood-brain barrier opening in Alzheimer’s disease with focused ultrasound
Focused Ultrasound for Addiction
In 2021, RNI led the world’s first human trial using focused ultrasound (FUS) technology for neuromodulation of patients suffering from substance use disorder. This non-invasive device can precisely target brain regions like the nucleus accumbens (NAc), the brain’s reward center, without surgery or implants. Patients in the trial had significant craving reduction and substance intake. They also actively participated in behavioral therapies, suggesting a holistic approach to recovery.
To confirm these promising findings, RNI is launching a randomized, double-blind, sham-controlled clinical trial in 2024. This research has the potential to revolutionize addiction treatment as a complementary tool and offer millions an effective pathway to healing.
Visit ClinicalTrials.gov for trial details
Download a fact sheet
LEARN MORE:
- Low-Intensity Focused Ultrasound Targeting the Bilateral Nucleus Accumbens as a Potential Treatment for Substance Use Disorder: A First-in-Human Report
- Low-intensity focused ultrasound targeting the nucleus accumbens as a potential treatment for substance use disorder: safety and feasibility clinical trial
Human Operating System (HOS)
Researchers and engineers at the RNI Innovation Center have developed a digital ecosystem called the Human Operating System (HOS) to provide real-time, personalized health and wellness monitoring. The HOS integrates data from multiple sources such as electronic medical records, wearable and other medical devices (smartwatches, rings, pills), and a customized companion phone app (RNI Health App) are combined so that the RNI’s Artificial Intelligence technology can provide individual insights and alerts to our patients.
Studies have explored the use of the HOS for the detection of viral symptoms, signs of stress and burnout, the risk of substance cravings or potential relapses, as well as changes in chronic pain such as migraines. This data allows the RNI team to provide personalized monitoring and predictive reports to patients while at home.
LEARN MORE:
- This Pill Tracks Your Vitals From the Inside
- Prediction of viral symptoms using wearable technology and artificial intelligence: A pilot study in healthcare workers
- First-in-human trial of an ingestible vitals-monitoring pill
- Identifying biomarkers of drug use recurrence using wearable device technologies and phone applications
Deep Brain Stimulation (DBS) for Addiction
Deep Brain Stimulation (DBS) is an FDA-approved medical procedure that involves creating two small holes in the skull and safely inserting tiny electrodes into a specific area of the brain. This procedure has been successfully used for over 25 years to treat patients with Parkinson’s disease. The RNI team has studied use of this technology for the treatment of substance use disorder by placing these electrodes in the reward center of the brain, the nucleus accumbens. Once implanted, the DBS device acts like a pacemaker for the brain, carrying electrical stimulation to that area and reducing drug cravings.
This study is no longer recruiting participants.
Brain-Computer Interface Research
In 2023, the RNI’s Department of Neurosurgery, in partnership with Precision Neuroscience Corporation, successfully completed five first-in-human procedures in a pilot clinical study of Precision Neuroscience’s neural implant system. The study was designed to record and map the brain’s activity in unprecedented detail, signaling a major step toward restoring meaningful function to millions of people suffering from neurological illnesses and disorders.
During the study, a team of RNI neurosurgeons led by Peter Konrad, M.D., Ph.D., chair of the Department of Neurosurgery, temporarily placed the Precision system, called the Layer 7 Cortical Interface, on the brain of a patient undergoing resection of a brain tumor. They safely deployed the implant onto the brain for a portion of the surgery, allowing it to read, record, and map electrical activity from the surface of the brain. The interface contains 1,024 tiny electrodes spanning an area of one square centimeter, embedded in a flexible film that conforms to the brain surface. The film is one-fifth the thickness of a human hair and is designed to be implanted and removed by neurosurgeons without damaging brain tissue.
LEARN MORE:
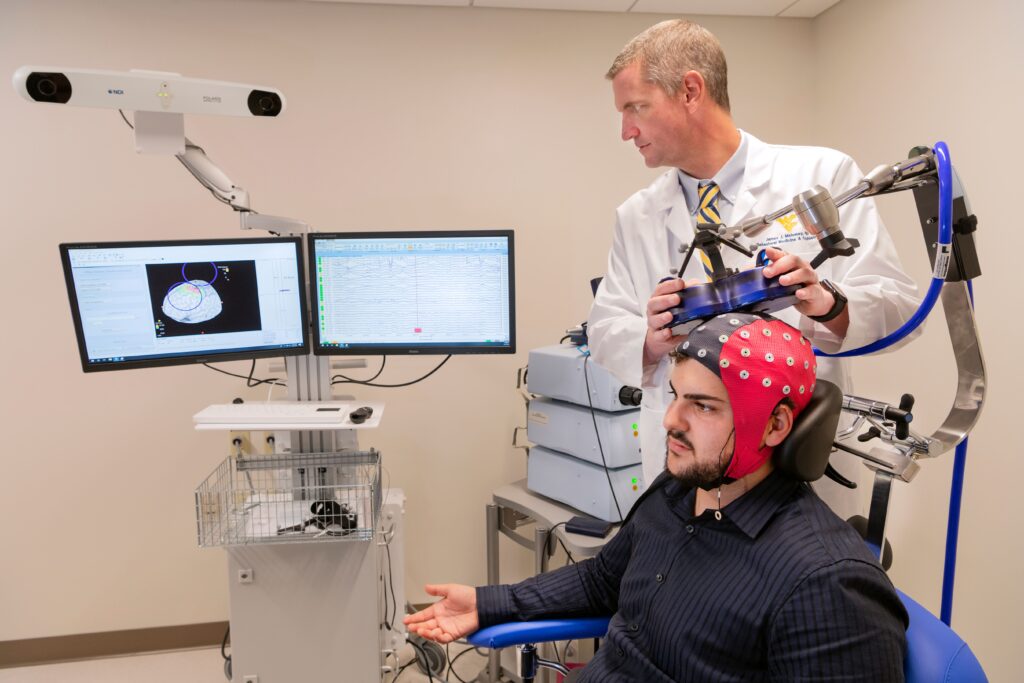
Transcranial Magnetic Stimulation (TMS)
Transcranial Magnetic Stimulation (TMS) is a non-invasive, FDA-approved therapeutic treatment that involves delivering a series of short magnetic pulses to targeted areas of the brain. Patients wear a specially designed cap for about 20 minutes while receiving treatment as the magnetic stimulation increases the neural activity in the targeted area. The treatment is most commonly used for patients with depression – but the RNI is conducting clinical trials to explore its applicability to other ailments such as addiction, chronic and acute pain, Alzheimer’s disease, and cognitive and motor skill impairment.
